Blog
Dealing With Cracked Heels
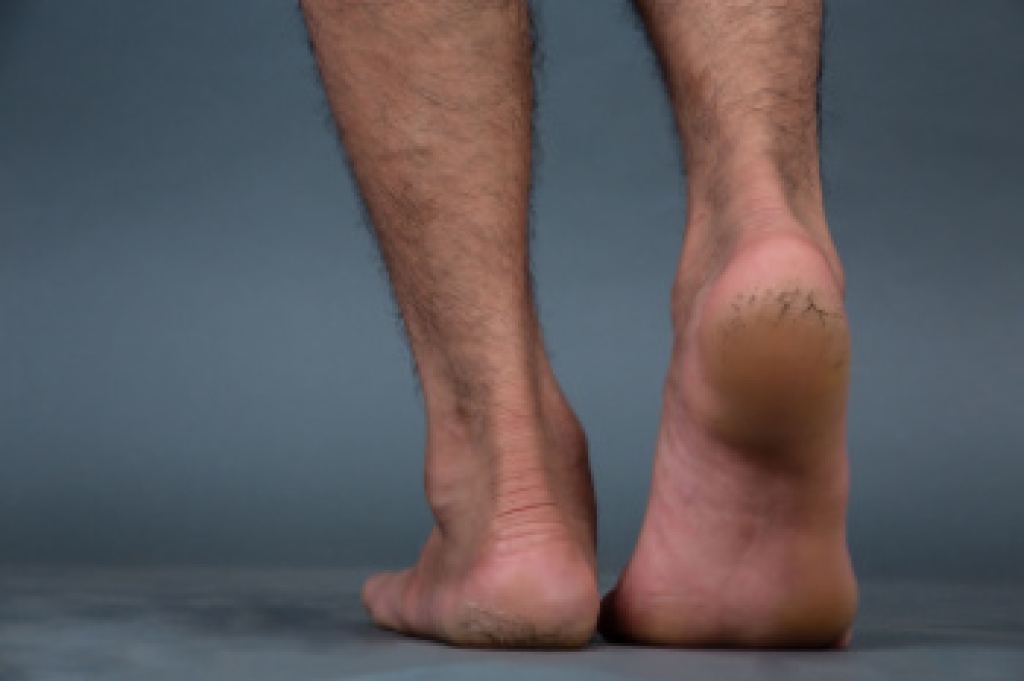
Cracked heels develop when the skin around the heel becomes dry, thick, and splits due to pressure and lack of moisture. Causes include prolonged standing, wearing open-back shoes, and footwear that does not properly support the heel, which increases stress on the skin. Dry climates can worsen the condition by removing natural moisture. Risk factors include obesity, aging, and poor foot-care habits. Symptoms include rough skin, flaking, discomfort, and painful fissures that can deepen if untreated. A podiatrist can assess severity, remove thickened skin safely, recommend treatments, and provide guidance on proper footwear and hydration. Cracked heels can be painful. If you have developed this condition, it is suggested that you consult a podiatrist who can offer effective treatment solutions, which may include prescribed medication.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact Jeffrey Parrett, DPM from Parrett Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Waxahachie, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Diabetes and How the Feet Are Affected
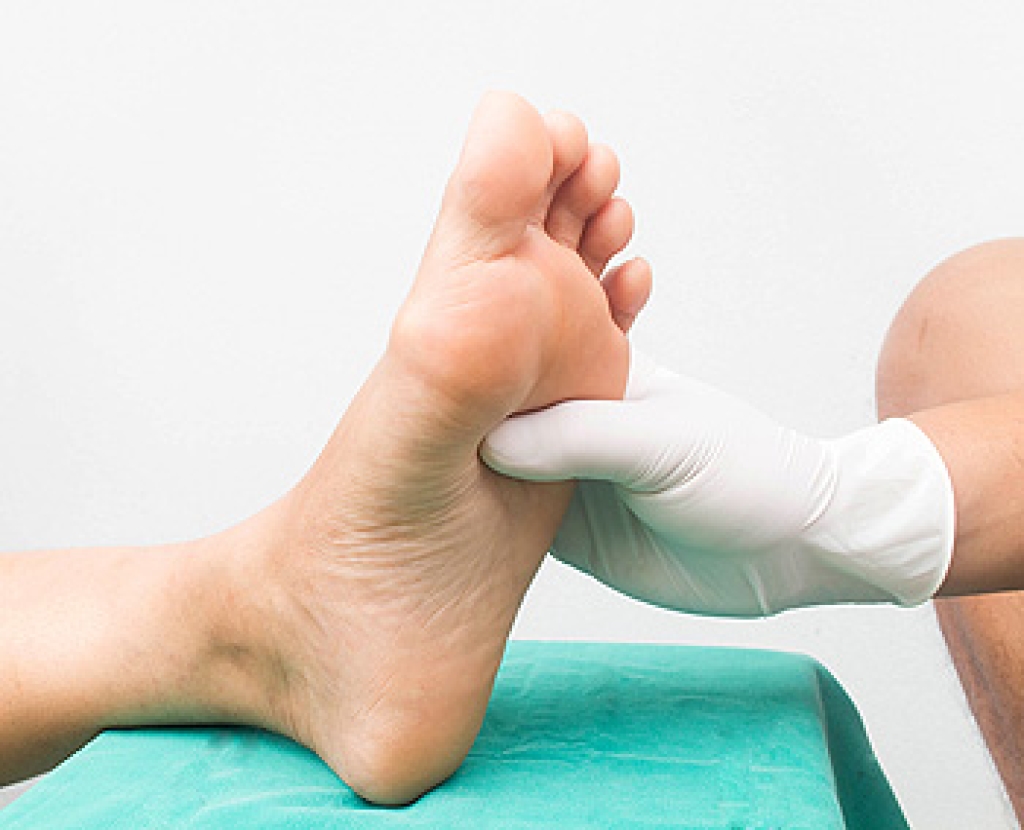
Diabetes is a chronic condition that affects how the body processes blood sugar and can have serious effects on foot health. Over time, it may cause nerve damage known as neuropathy, leading to reduced sensation in the feet. Poor circulation can also develop, slowing healing and increasing the risk of complications. Individuals may experience foot ulcers, blisters, pain, and infections that can worsen without proper care. Risk factors include prolonged high blood sugar levels, poor foot hygiene, and wearing ill-fitting footwear. A podiatrist can help by monitoring foot health, treating wounds, and providing guidance on proper care and prevention. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can help you to manage this serious condition.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Jeffrey Parrett, DPM from Parrett Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions, please feel free to contact our office located in Waxahachie, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
When Foot Pain May Indicate Arthritis

Foot pain can occur after long hours of standing, sports activity, or wearing shoes that do not fit well. Sometimes the pain improves, but ongoing discomfort may be a sign of arthritis. This inflammatory joint condition causes swelling, stiffness, and reduced movement. The foot has many small joints that help support body weight and allow smooth walking. When arthritis affects these joints, pain may worsen with activity or after periods of rest. Osteoarthritis develops when cartilage, the smooth tissue that cushions bones, gradually wears away. Other forms, such as rheumatoid arthritis and psoriatic arthritis, occur when the immune system attacks joint tissue. Gout is another type of arthritis that causes sudden, intense pain when crystal deposits form in a joint, often in the big toe. A podiatrist can identify the cause of foot pain, assess joint damage, and recommend medical treatment to improve comfort and walking ability. If you are experiencing foot pain, it is suggested that you make an appointment with a podiatrist.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Jeffrey Parrett, DPM from Parrett Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions please feel free to contact our office located in Waxahachie, TX . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
How the Body Repairs a Foot Wound
When the skin on the foot is injured, the body begins a complex healing response designed to close the wound and restore healthy tissue. This process happens in several connected stages that gradually rebuild the damaged area. First, the body works to stop bleeding and protect the injury. Blood cells gather at the site and form a clot that seals the wound, preventing harmful bacteria from entering. Next, the body begins building new tissue. Fresh cells grow, small blood vessels develop, and the wound slowly fills in as healthy skin forms. During the final stage, the new tissue strengthens and becomes more organized. The skin becomes firmer and better able to handle normal pressure from standing and walking. Proper wound care, cleanliness, and reduced pressure help support healing. If a foot wound heals slowly or shows signs of infection, it is suggested that you promptly see a podiatrist for a proper diagnosis and appropriate treatment.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Jeffrey Parrett, DPM from Parrett Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions please contact our office located in Waxahachie, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

